|
Graft-host vascularization occurred in 2 (12%) eyes. There was no formation of ''secondary anterior chamber'' postoperatively. These eyes were managed by injection of air or a mixture of perfluoropropane (C3F8) with air (14% C3F8, 86% air) into the anterior chamber to temporarily seal the microperforations. 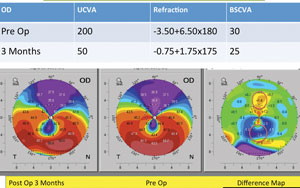
However, this perforation had no statistical impact on final visual acuity (p = 0.47). Intraoperative perforation of DM during DALK occurred in 2 (12%) eyes. However, crossing the two groups using the Mann Whitney test showed no statistical difference between groups (p = 0.40). This analysis indicated that astigmatism correction was statistically significant with the big bubble technique (p = 0.008) compared to manual dissection (p = 0.056). The cohort was subdivided into 2 groups based on the surgical technique and the analysis was repeated. Visual acuity increased statistically significantly from 0.9 ± 0.3 (range 0.5-1.6) preoperatively to 0.4 ± 0.2 (range 0.0-0.7) at last follow-up (p 0.05, all cases) (Table 2). The mean overall age was 31.4 ± 9.6 years (range, 1950 years). Results: The mean follow up was 14.6 ± 8.2 months (range 6-35 months). Visual acuity (Log-MAR notation), intraocular pressure, intraoperative complications and postoperative graft status were assessed. The big bubble technique was performed in 10 (62.5%) eyes and manual dissection was performed in the remaining 6 (37.5%) eyes. Baring of Descemet's membrane (DM) during DALK was achieved in 8 (50%) eyes residual stroma was left intraoperatively in the remaining 8 (50%) eyes. Methods: A retrospective review was performed in 16 eyes of 16 patients who underwent DALK at the King Khaled Eye Specialist Hospital, Riyadh, Saudi Arabia between Januand December 30, 2009. Purpose: To present the surgical outcomes of deep anterior lamellar keratoplasty (DALK) for pellucid marginal degeneration (PMD). Saudi Journal of Ophthalmology (2013) 27, 11-14ĭeep anterior lamellar keratoplasty for pellucid marginal degeneration The main graft-related complication was graft–host vascularization (2/16 eyes).ĭALK reduces severe corneal astigmatism and results in good visual and refractive outcomes and is an effective alternative for patients with PMD. 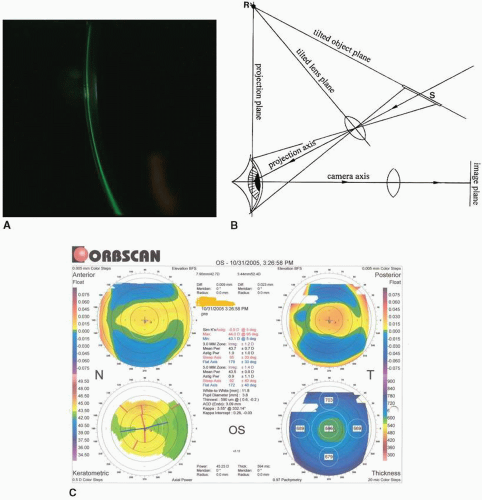
Postoperative visual acuity was not statistically significantly related to gender, type of surgical technique, and baring or perforation of DM. <0.02, respectively) compared to preoperative. 
There was a statistically significant improvement in postoperative sphere, cylinder, and spherical equivalent (p Visual acuity increased statistically significantly from 0.9☐.3 (range 0.5–1.6) preoperatively to 0.4☐.2 (range 0.0–0.7) at last follow-up (p The mean overall age was 31.4☙.6years (range, 19–50years). The mean follow up was 14.6☘.2months (range 6–35months). Visual acuity (LogMAR notation), intraocular pressure, intraoperative complications and postoperative graft status were assessed. Baring of Descemet’s membrane (DM) during DALK was achieved in 8 (50%) eyes residual stroma was left intraoperatively in the remaining 8 (50%) eyes. To present the surgical outcomes of deep anterior lamellar keratoplasty (DALK) for pellucid marginal degeneration (PMD).Ī retrospective review was performed in 16 eyes of 16 patients who underwent DALK at the King Khaled Eye Specialist Hospital, Riyadh, Saudi Arabia between Januand December 30, 2009. Abstract of research paper on Clinical medicine, author of scientific article - Abdullah A.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
